Government crackdown and legal entanglements take all the fun out of the Medicare Advantage plan bonanza.
By Wolf Richter for WOLF STREET.
Humana is one of the big health insures with Medicare Advantage Plans that have come under intense scrutiny from this Administration, from the prior administration, from Congress, from legal actions, and from investigative reports in the media, amid allegations of dramatically overbilling Medicare. These insurers are facing a full-blown government crackdown.
But it was so sweet while it lasted, generating huge profits, big revenue gains, and a massive run-up of the price of the stock: Humana’s shares – along with others in that arena – shot higher and higher from 2017 through 2022. But amid that crackdown, revenue growth has stalled over the past few quarters, and Humana posted a big loss in February.
Humana’s shares [HUM], which started cratering in November 2022, have now entered our pantheon of Imploded Stocks, for which the minimum requirement is a plunge of 70% from the more or less recent all-time high. Its shares today fell 1.8% to $166.01, down by 71% from the all-time high on November 3, 2022, and down by 37% from a year ago, and pretty exactly back where they’d first been 11 years ago, in March 2015 (data via YCharts).
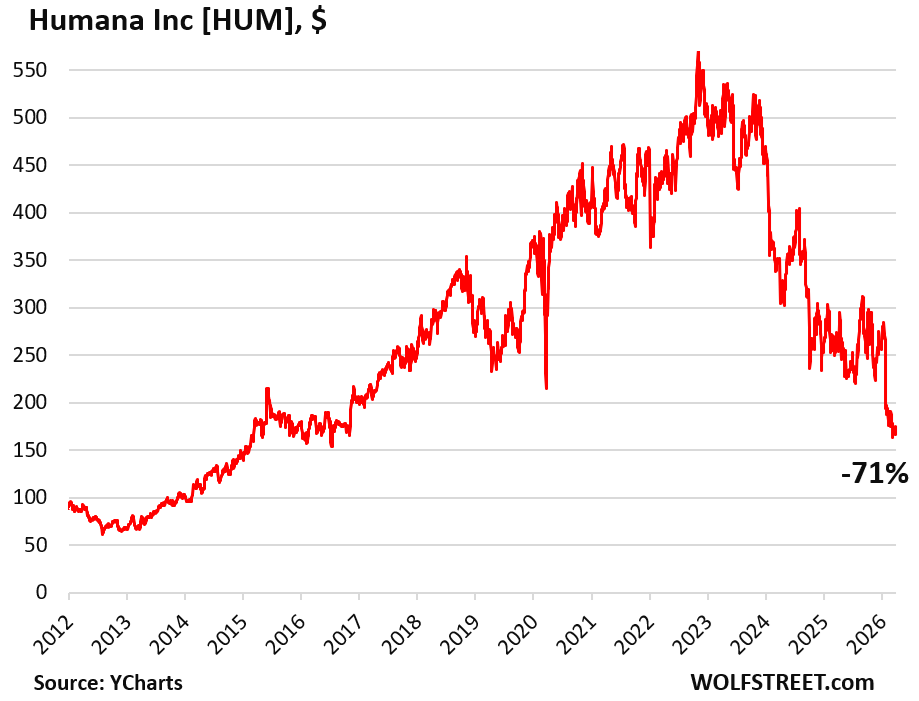
This is what happens when corporate revenue growth, profits, bonuses, and lucrative stock-based compensation plans depend on overbilling the government, and the government finally belatedly gets tired of it, and cracks down.
Medicare Advantage plans are a semi-privatization of Medicare under which the government pays the health insurer a monthly amount for each of their enrollees, and the insurer then pays for the treatment of the enrollee (the enrollee pays for Medicare Part B and some also pay a premium for the Advantage Plan). Advantage Plans include prescription drug benefits and assorted other benefits, caps, and reductions.
The monthly amount that the government pays to the insurer for each enrollee rises with the health problems the enrollee has. So, inevitably… if the insurer “finds” more and bigger health problems, or exaggerates existing health problems, they can claim substantially higher monthly fees, even if those health problems don’t exist, or never get treated. And the government pays them for it.
This type of overbilling led to higher costs for Medicare, and part of those were passed on and led to higher Medicare Part B premiums that seniors pay. According to a report by the US Congress Joint Economic Committee earlier in March, “in 2025 the federal government paid Medicare Advantage insurers an estimated $76 billion to $84 billion more than it would have cost to cover the same beneficiaries in Traditional Medicare.”
The committee found that “overpayments increased Part B premiums by $212 per enrollee in 2025, totaling $13.4 billion in higher premiums.”
And it found that since 2016, these overpayments “have added an estimated $82 billion to Part B premiums.”
But every dollar that was overpaid by the government added to the revenues and profits of the insurers. And the incredible trajectory of their stocks from 2017 through 2022 shows that.
And there are other aspects, as the Medicare overbilling scandal has metastasized. For example, a federal court ruled last week that Humana, CVS Health subsidiary Aetna, and Elevance Health, must face a civil lawsuit that alleges, based on a whistleblower that came forward in 2021, that the insurers paid “hundreds of millions” in kickbacks between 2016 and 2021 to online brokerages to steer people to their Medicare Advantage plans – because those Advantage Plans were so immensely lucrative to the insurers.
Humana has also gotten caught up in allegations that it had been overbilling the government for Medicare Part D (prescription drugs) plans, and settled a number of those cases, including for $90 million in 2024, a whistleblower case brought by one of its former actuaries.
But as far as investors and Wall Street analysts are concerned, the bigger the Medicare overbilling, the better because it made everyone a lot of money. Just don’t get caught.
Enjoy reading WOLF STREET and want to support it? You can donate. I appreciate it immensely. Click on the mug to find out how:
![]()


THANKS for helping put the spotlight on these egregious MedicareAdvantage Plan practices. It really is scandalous and sad.
Just like the fraud in MN, CA and elsewhere in various gov’t connected programs…this graft has been going on for a long time.
Gov’t is and has been part of the problem: both from management and oversight povs.
Thanks wolf
Are there any good providers of this stuff?
Time for a slap on the wrist.
Fraud of this magnitude will probably force the board of directors to cut CEO’s bonus by 20%.
Forget that, if they know how to look out for #1 then investors reward you!
Haha
You know just don’t go full Nahhhzeee, never go full Nahhhzeeee 😂
…plus a pardon and lobbying gig.
Those of us who have been to places with national healthcare like Taiwan know the benefits. These plans work because of caps on medical procedures, doctor’s visits, imaging/diagnostics, and medicine all of which are nonstarters in the US because of profiteering.
Lastly, tover 40% of the US population is obese. Diabetes, obesity, and blood pressure are lifestyle diseases that waste resources on people who choose to be unhealthy. Why should we subsidize their behavior?
Howdy Youngins. Always pay attention to every credit card charge. Humana also charges credit cards yearly renewal fees for policies that did not exist. BOA card services makes it extremely difficult for the card holder that notifies them about fraudulent charges. They protect the merchant first…Long wait times for customer service centers …. Certain claims must be called in and you will wait and wait and wait…..
As a former Humana actuary (unfortunately, I am not the aforementioned whistleblower), this is not at all surprising. I’d love to see a study that shows what portion of healthcare spending goes where – @Wolf let me know if I can help! I would bet the amount that goes to doctors and actual providers of care (not admin/IT/coding staff at the hospital conglomerates) has got to be a laughably small percentage, if not a rounding error.
The whole system is broken way beyond repair and this is just one tiny example of how the industry is set up to scrape every last extra dollar possible out of the system for as long as possible.
The good news is that health insurance is so convoluted that not even AI can take away those jobs :D
Any system needs a certain amount of operational types to make sure there are facilities, equipment, etc and that the highly skilled are properly compensated. Like oil in an engine. Unfortunately, too many of these people think they are the engine when they really are just mucking it up.